
Overtreatment with drugs kills many people, and the death rate is increasing. It is therefore strange that we have allowed this long-lasting drug pandemic to continue, and even more so because most of the drug deaths are easily preventable.
In 2013, I estimated that our prescription drugs are the third leading cause of death after heart disease and cancer,1 and in 2015, that psychiatric drugs alone are also the third leading cause of death.2 However, in the US, it is commonly stated that our drugs are "only" the fourth leading cause of death.3,4 This estimate was derived from a 1998 meta-analysis of 39 US studies where monitors recorded all adverse drug reactions that occurred while the patients were in hospital, or which were the reason for hospital admission.5
This methodology clearly underestimates drug deaths. Most people who are killed by their drugs die outside hospitals, and the time people spent in hospitals was only 11 days on average in the meta-analysis.5 Moreover, the meta-analysis only included patients who died from drugs that were properly prescribed, not those who died as a result of errors in drug administration, noncompliance, overdose, or drug abuse, and not deaths where the adverse drug reaction was only possible.5
Many people die because of errors, e.g. simultaneous use of contraindicated drugs, and many possible drug deaths are real. Moreover, most of the included studies are very old, the median publication year being 1973, and drug deaths have increased dramatically over the last 50 years. As an example, 37,309 drug deaths were reported to the FDA in 2006 and 123,927 ten years later, which is 3.3 times as many.6
In hospital records and coroners' reports, deaths linked to prescription drugs are often considered to be from natural or unknown causes. This misconception is particularly common for deaths caused by psychiatric drugs.2,7 Even when young patients with schizophrenia suddenly drop dead, it is called a natural death. But it is not natural to die young and it is well known that neuroleptics can cause lethal heart arrhythmias.
Many people die from the drugs they take without raising any suspicion that it could be an adverse drug effect. Depression drugs kill many people, mainly among the elderly, because they can cause orthostatic hypotension, sedation, confusion, and dizziness. The drugs double the risk of falls and hip fractures in a dose-dependent manner,8,9 and within one year after a hip fracture, about one-fifth of the patients will have died. As elderly people often fall anyway, it is not possible to know if such deaths are drug deaths.
Another example of unrecognised drug deaths is provided by non-steroidal anti-inflammatory drugs (NSAIDs). They have killed hundreds of thousands of people,1 mainly through heart attacks and bleeding stomach ulcers, but these deaths are unlikely to be coded as adverse drug reactions, as such deaths also occur in patients who do not take the drugs.
The 1998 US meta-analysis estimated that 106,000 patients die every year in hospital because of adverse drug effects (a 0.32% death rate).5 A carefully done Norwegian study examined 732 deaths that occurred in a two-year period ending in 1995 at a department of internal medicine, and it found that there were 9.5 drug deaths per 1,000 patients (a 1% death rate).10 This is a much more reliable estimate, as drug deaths have increased markedly. If we apply this estimate to the US, we get 315,000 annual drug deaths in hospitals. A review of four newer studies, from 2008 to 2011, estimated that there were over 400,000 drug deaths in US hospitals.11
Drug usage is now so common that newborns in 2019 could be expected to take prescription drugs for roughly half their lives in the US.12 Moreover, polypharmacy has been increasing.12
How Many People Are Killed by Psychiatric Drugs?
If we want to estimate the death toll of psychiatric drugs, the most reliable evidence we have are the placebo-controlled randomised trials. But we need to consider their limitations.
First, they usually run for only a few weeks even though most patients take the drugs for many years.13,14
Second, polypharmacy is common in psychiatry, and this increases the risk of dying. As an example, the Danish Board of Health has warned that adding a benzodiazepine to a neuroleptic increases mortality by 50-65%.15
Third, half of all deaths are missing in published trial reports.16 For dementia, published data show that for every 100 people treated with a newer neuroleptic for ten weeks, one patient is killed.17 This is an extremely high death rate for a drug, but FDA data on the same trials show it is twice as high, namely two patients killed per 100 after ten weeks.18 And if we extend the observation period, the death toll becomes even higher. A Finnish study of 70,718 community-dwellers newly diagnosed with Alzheimer's disease reported that neuroleptics kill 4-5 people per 100 annually compared to patients who were not treated.19
Fourth, the design of psychiatric drug trials is biased. In almost all cases, patients were already in treatment before they entered the trial,2,7 and some of those randomised to placebo will therefore experience withdrawal effects that will increase their risk of dying, e.g. because of akathisia. It is not possible to use the placebo-controlled trials in schizophrenia to estimate the effect of neuroleptics on mortality because of the drug withdrawal design. The suicide rate in these unethical trials was 2-5 times higher than the norm.20,21 One in every 145 patients who entered the trials of risperidone, olanzapine, quetiapine, and sertindole died, but none of these deaths were mentioned in the scientific literature, and the FDA didn't require them to be mentioned.
Fifth, events after the trial is stopped are ignored. In Pfizer's trials of sertraline in adults, the risk ratio for suicides and suicide attempts was 0.52 when the follow-up was only 24 hours, but 1.47 when the follow-up was 30 days, i.e. an increase in suicidal events.22 And when researchers reanalysed the FDA trial data on depression drugs and included harms occurring during followup, they found that the drugs double the number of suicides in adults compared to placebo.23,24
In 2013, I estimated that, in people aged 65 and above, neuroleptics, benzodiazepines, or similar, and depression drugs kill 209,000 people annually in the United States.2 I used rather conservative estimates, however, and usage data from Denmark, which are far lower than those in the US. I have therefore updated the analysis based on US usage data, again focusing on older age groups.
For neuroleptics, I used the estimate of 2% mortality from the FDA data.18
For benzodiazepines and similar drugs, a matched cohort study showed that the drugs doubled the death rate, although the average age of the patients was only 55.25 The excess death rate was about 1% per year. In another large, matched cohort study, the appendix to the study report shows that hypnotics quadrupled the death rate (hazard ratio 4.5).26 These authors estimated that sleeping pills kill between 320,000 and 507,000 Americans every year.26 A reasonable estimate of the annual death rate would therefore be 2%.
For SSRIs, a UK cohort study of 60,746 depressed patients older than 65 showed that they led to falls and that the drugs kill 3.6% of patients treated for one year.27 The study was done very well, e.g. the patients were their own control in one of the analyses, which is a good way to remove the effect of confounders. But the death rate is surprisingly high.
Another cohort study, of 136,293 American postmenopausal women (age 50-79) participating in the Women's Health Initiative study, found that depression drugs were associated with a 32% increase in all-cause mortality after adjustment for confounding factors, which corresponded to 0.5% of women killed by SSRIs when treated for one year.28 The death rate was very likely underestimated. The authors warned that their results should be interpreted with great caution, as the way exposure to antidepressant drugs was ascertained carried a high risk of misclassification, which would make it more difficult to find an increase in mortality. Further, the patients were much younger than in the UK study, and the death rate increased markedly with age and was 1.4% for those aged 70-79. Finally, the exposed and unexposed women were different for many important risk factors for early death, whereas the people in the UK cohort were their own control.
For these reasons, I decided to use the average of the two estimates, a 2% annual death rate.
These are my results for the US for these three drug groups for people at least 65 years of age (58.2 million; usage is in outpatients only):29-32
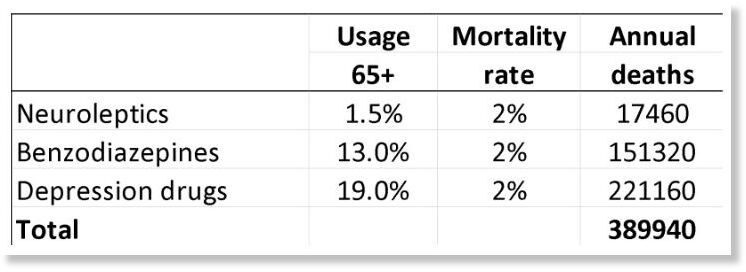
On the other hand, the data on death rates come from studies where many patients were also on several psychiatric drugs in the comparison group, so this is not likely to be a major limitation considering also that polypharmacy increases mortality beyond what the individual drugs cause.
Statistics from the Centers for Disease Control and Prevention list these four top causes of death:33
Heart disease: 695,547
Cancer: 605,213
Covid-19: 416,893
Accidents: 224,935
Covid-19 deaths are rapidly declining, and many such deaths are not caused by the virus but merely occurred in people who tested positive for it because the WHO advised that all deaths in people who tested positive should be called Covid deaths.
Young people have a much smaller death risk than the elderly, as they rarely fall and break their hip, which is why I have focused on the elderly. I have tried to be conservative. My estimate misses many drug deaths in those younger than 65 years; it only included three classes of psychiatric drugs; and it did not include hospital deaths.
I therefore do not doubt that psychiatric drugs are the third leading cause of death after heart disease and cancer.
Other Drug Groups and Hospital Deaths
Analgesics are also major killers. In the US, about 70,000 people were killed in 2021 by an overdose of a synthetic opioid.34
The usage of NSAIDs is also high. In the US, 26% of adults use them regularly, 16% of which get them without a prescription35 (mostly ibuprofen and diclofenac).36
As there seems to be no major differences between the drugs in their capacity to cause thromboses,37 we may use data for rofecoxib. Merck and Pfizer underreported thrombotic events in their trials of rofecoxib and celecoxib, respectively, to such an extent that it constituted fraud,1 but in one trial, of colorectal adenomas, Merck assessed thrombotic events. There were 1.5 more cases of myocardial infarction, sudden cardiac death or stroke on rofecoxib than on placebo per 100 patients treated.38 About 10% of the thromboses are fatal, but heart attacks are rare in young people. Restricting the analysis to those aged at least 65, we get 87,300 annual deaths.
It has been estimated that 3,700 deaths occur each year in the UK due to peptic ulcer complications in NSAID users,39 corresponding to about 20,000 deaths each year in the US. Thus, the total estimate of NSAID deaths is about 107,000.
If we add the estimates above, 315,000 hospital deaths, 390,000 psychiatric drug deaths, 70,000 synthetic opioid deaths, and 107,000 NSAID deaths, we get 882,000 drug deaths in the United States annually.
Many commonly used drugs other than those mentioned above can cause dizziness and falls, e.g. anticholinergic drugs against urinary incontinence and dementia drugs, which are used by 1% and 0.5% of the Danish population, respectively, even though they do not have any clinically relevant effects.1,2
It is difficult to know what the exact death toll of our drugs is, but there can be no doubt that they are the leading cause of death. And the death toll would be much higher if we included people below 65 years of age. Moreover, from the official number of deaths from heart disease, we would need to subtract those caused by NSAIDs, and from accidents, deaths by falls caused by psychiatric drugs and many other drugs.
If such a hugely lethal pandemic had been caused by a microorganism, we would have done everything we could to get it under control. The tragedy is that we could easily get our drug pandemic under control, but when our politicians act, they usually make matters worse. They have been so heavily lobbied by the drug industry that drug regulation has become much more permissive than it was in the past.40
Most of the drug deaths are preventable,41 above all because most of the patients who died didn't need the drug that killed them. In placebo-controlled trials, the effect of neuroleptics and depression drugs has been considerably below the least clinically relevant effect, also for very severe depression.2,7 And, despite their name, non-steroidal, anti-inflammatory drugs, NSAIDs do not have anti-inflammatory effects,1,42 and systematic reviews have shown that their analgesic effect is similar to that of paracetamol (acetaminophen). Yet, most patients with pain are recommended to take both paracetamol and an NSAID over the counter. This will not increase the effect, only the risk of dying.
Most tragically, leading psychiatrists all over the world do not realise how ineffective and dangerous their drugs are. A US psychiatrist, Roy Perlis, professor at Harvard, argued in April 2024 that depression pills should be sold over the counter because they are "safe and effective."43 They are highly unsafe and ineffective. Perlis also claimed that depression drugs do not increase the risk of suicide in people older than 25, which is also wrong. They double suicides in adults.23,24
Perlis wrote, "Some still question the biological basis of this disorder, despite the identification of more than 100 genes that increase depression risk and neuroimaging studies showing differences in the brains of people with depression." Both of these claims are plain wrong. Genetic association studies have come up empty-handed and so have brain imaging studies, which are generally highly flawed.44 People are depressed because they live depressing lives, not because of some brain disorder.
References
1 Gøtzsche PC. Deadly Medicines and Organised Crime: How Big Pharma Has Corrupted Health Care. London: Radcliffe Publishing; 2013.
2 Gøtzsche PC. Deadly Psychiatry and Organised Denial. Copenhagen: People's Press; 2015.
3 Schroeder MO. Death by Prescription: By one estimate, taking prescribed medications is the fourth leading cause of death among Americans. US News 2016; Sept 27.
4 Light DW, Lexchin J, Darrow JJ. Institutional corruption of pharmaceuticals and the myth of safe and effective drugs. J Law Med Ethics 2013;41:590-600.
5 Lazarou J, Pomeranz BH, Corey PN. Incidence of adverse drug reactions in hospitalized patients: a meta-analysis of prospective studies. JAMA 1998;279:1200-5.
6 FAERS Reporting by Patient Outcomes by Year. FDA 2015;Nov 10.
7 Gøtzsche PC. Mental Health Survival Kit and Withdrawal From Psychiatric Drugs. Ann Arbor: L H Press; 2022.
8 Hubbard R, Farrington P, Smith C, et al. Exposure to tricyclic and selective serotonin reuptake inhibitor antidepressants and the risk of hip fracture. Am J Epidemiol 2003;158:77-84.
9 Thapa PB, Gideon P, Cost TW, et al. Antidepressants and the risk of falls among nursing home residents. N Engl J Med 1998;339:875-82.
10 Ebbesen J, Buajordet I, Erikssen J, et al. Drug-related deaths in a department of internal medicine. Arch Intern Med 2001;161:2317-23.
11 James JTA. A new, evidence-based estimate of patient harms associated with hospital care. J Patient Saf 2013;9:122-8.
12 Ho JY. Life Course Patterns of Prescription Drug Use in the United States. Demography 2023;60:1549-79.
13 Gøtzsche PC. Long-term use of antipsychotics and antidepressants is not evidence-based. Int J Risk Saf Med 2020;31:37-42.
14 Gøtzsche PC. Long-Term Use of Benzodiazepines, Stimulants and Lithium is Not Evidence-Based. Clin Neuropsychiatry 2020;17:281-3.
15 Forbruget af antipsykotika blandt 18-64 årige patienter, med skizofreni, mani eller bipolar affektiv sindslidelse. København: Sundhedsstyrelsen; 2006.
16 Hughes S, Cohen D, Jaggi R. Differences in reporting serious adverse events in industry sponsored clinical trial registries and journal articles on antidepressant and antipsychotic drugs: a cross-sectional study. BMJ Open 2014;4:e005535.
17 Schneider LS, Dagerman KS, Insel P. Risk of death with atypical antipsychotic drug treatment for dementia: meta-analysis of randomized placebo-controlled trials. JAMA 2005;294:1934-43.
18 FDA package insert for Risperdal (risperidone). Accessed 30 May 2022.
19 Koponen M, Taipale H, Lavikainen P, et al. Risk of Mortality Associated with Antipsychotic Monotherapy and Polypharmacy Among Community-Dwelling Persons with Alzheimer's Disease. J Alzheimers Dis 2017;56:107-18.
20 Whitaker R. Lure of Riches Fuels Testing. Boston Globe 1998; Nov 17.
21 Whitaker R. Mad in America: Bad science, Bad medicine, and the Enduring Mistreatment of the Mentally Ill. Cambridge: Perseus Books Group; 2002:page 269.
22 Vanderburg DG, Batzar E, Fogel I, et al. A pooled analysis of suicidality in double-blind, placebo-controlled studies of sertraline in adults. J Clin Psychiatry 2009;70:674-83.
23 Hengartner MP, Plöderl M. Newer-Generation Antidepressants and Suicide Risk in Randomized Controlled Trials: a Re-Analysis of the FDA Database. Psychother Psychosom 2019;88:247-8.
24 Hengartner MP, Plöderl M. Reply to the Letter to the Editor: "Newer-Generation Antidepressants and Suicide Risk: Thoughts on Hengartner and Plöderl's ReAnalysis." Psychother Psychosom 2019;88:373-4.
25 Weich S, Pearce HL, Croft P, et al. Effect of anxiolytic and hypnotic drug prescriptions on mortality hazards: retrospective cohort study. BMJ 2014;348:g1996.
26 Kripke DF, Langer RD, Kline LE. Hypnotics' association with mortality or cancer: a matched cohort study. BMJ Open 2012;2:e000850.
27 Coupland C, Dhiman P, Morriss R, et al. Antidepressant use and risk of adverse outcomes in older people: population based cohort study. BMJ 2011;343:d4551.
28 Smoller JW, Allison M, Cochrane BB, et al. Antidepressant use and risk of incident cardiovascular morbidity and mortality among postmenopausal women in the Women's Health Initiative study. Arch Intern Med 2009;169:2128-39.
29 O'Neill A. Age distribution in the United States from 2012 to 2022. Statista 2024;Jan 25.
30 Olfson M, King M, Schoenbaum M. Antipsychotic Treatment of Adults in the United States. Psychiatrist.com 2015;Oct 21.
31 Maust DT, Lin LA, Blow FC. Benzodiazepine Use and Misuse Among Adults in the United States. Psychiatr Serv 2019;70:97-106.
32 Brody DJ, Gu Q. Antidepressant Use Among Adults: United States, 2015-2018. CDC 2020; Sept.
33 Centers for Disease Control and Prevention. Leading Causes of Death. 2024; Jan 17.
34 Drug Overdose Deaths. Centers for Disease Control and Prevention 2023; Aug 22.
35 Davis JS, Lee HY, Kim J, et al. Use of non-steroidal anti-inflammatory drugs in US adults: changes over time and by demographic. Open Heart 2017;4:e000550.
36 Conaghan PG. A turbulent decade for NSAIDs: update on current concepts of classification, epidemiology, comparative efficacy, and toxicity. Rheumatol Int 2012;32:1491-502.
37 Bally M, Dendukuri N, Rich B, et al. Risk of acute myocardial infarction with NSAIDs in real world use: bayesian meta-analysis of individual patient data. BMJ 2017;357:j1909.
38 Bresalier RS, Sandler RS, Quan H, et al. Cardiovascular Events Associated with Rofecoxib in a Colorectal Adenoma Chemoprevention Trial. N Engl J Med 2005;352:1092-102.
39 Blower AL, Brooks A, Fenn GC, et al. Emergency admissions for upper gastrointestinal disease and their relation to NSAID use. Aliment Pharmacol Ther 1997;11:283-91.
40 Davis C, Lexchin J, Jefferson T, Gøtzsche P, McKee M. "Adaptive pathways" to drug authorisation: adapting to industry? BMJ 2016;354:i4437.
41 van der Hooft CS, Sturkenboom MC, van Grootheest K, et al. Adverse drug reaction-related hospitalisations: a nationwide study in The Netherlands. Drug Saf 2006;29:161-8.
42 Gøtzsche PC. Big marketing hoax: Non-steroidal, anti-inflammatory drugs (NSAIDs) are not anti-inflammatory. Copenhagen: Institute for Scientific Freedom 2022;Nov 10.
43 Perlis R. The time has come for over-the-counter antidepressants. Stat News 2024;April 8.
44 Gøtzsche PC. Critical Psychiatry Textbook. Copenhagen: Institute for Scientific Freedom; 2022. Freely available.
Dr. Peter Gøtzsche co-founded the Cochrane Collaboration, once considered the world's preeminent independent medical research organization. In 2010 Gøtzsche was named Professor of Clinical Research Design and Analysis at the University of Copenhagen. Gøtzsche has published more than 97 papers in the "big five" medical journals (JAMA, Lancet, New England Journal of Medicine, British Medical Journal, and Annals of Internal Medicine). Gøtzsche has also authored books on medical issues including Deadly Medicines and Organized Crime. Following many years of being an outspoken critic of the corruption of science by pharmaceutical companies, Gøtzsche's membership on the governing board of Cochrane was terminated by its Board of Trustees in September, 2018. Four board resigned in protest.
Source link

